Heroes in Our Community
Amid pandemic, UPrep parents play critical roles
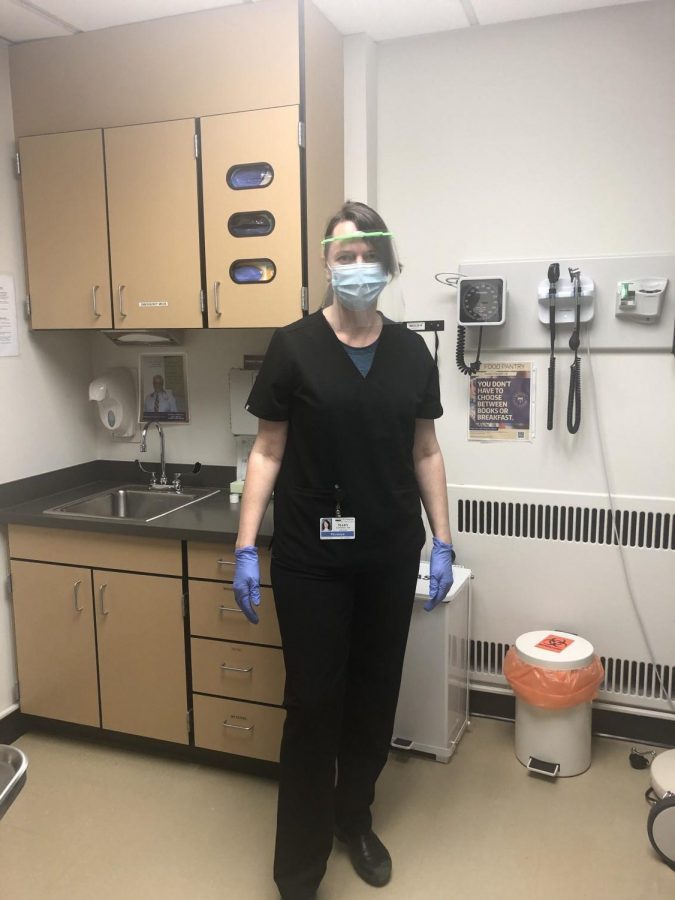
Photo: Dr. Alice Franck
Mollie Kauffman, head of primary and same-day care at a University of Washington clinic, wears a mask, face shield and gloves to evaluate a patient with respiratory symptoms. Kauffman is one of several UPrep parents working in the fight against COVID-19.
From enforced social distancing to shuttered businesses and spiking death tolls, COVID-19 has interrupted daily life across society. Few, however, are in a professional position to directly partake in the fight against the virus.
Some University Prep parents are playing important roles in the movement to stop the spread of COVID-19.
Carl Bergstrom, a professor of biology at the University of Washington and parent of two UPrep students, has studied both infectious diseases and the spread of misinformation on social networks for many years.
These two topics recently connected during the COVID-19 pandemic. Bergstrom is teaching a course to undergraduate students, and he has adapted it to be about the virus. He has been using testing and mathematical modeling to learn more about controlling the spread of the disease.
“[I’ve been] working with economists and people doing the tech side to figure out how we can roll out large-scale testing in the U.S,” Bergstrom said.
He is happy that his work is proving to be useful.
“Most of the time, when you’re doing science, you’re doing these narrow things,” Bergstrom said. “There are occasionally periods where what you’re doing becomes enormously important to the public and to society.”
Mollie Kauffman is also a UPrep parent. She is the head of primary and same-day care at Hall Health Center, a clinic primarily for students at the University of Washington. The clinic has now shifted how it sees patients.
It is now common for health facilities to have “COVID-only” areas. Kauffman’s office still provides same-day care but has dedicated a separate area to patients with COVID-19 symptoms. She sees fewer patients now that fewer students are on campus, prompting her office to begin telemedicine on Zoom.
“We’ve actually been able to do a lot with the Zoom visits, and it’s been good to keep people out of the office,” Kauffman said. “It’s an important social distancing role for our patients.”
While medical workers understand the need to change ways of normal life, they struggle to convince others of the same.
Bergstrom believes when people understand more about the virus, they’re more willing to play their part to keep everyone safe.
“Communicating about public health is doing public health,” he said.
Kauffman agrees with Bergstrom that communication is key during this time.
“Some of [the spread of misinformation] is natural with a new illness. But I also think there’s a lot of fear,” she said. “Whether people have an agenda to put [misinformation] out or whether it’s just confusion and lack of knowledge, it’s sometimes hard to tell.”
Bergstrom believes that people should read information from one quality source each day, as overconsumption of media is unnecessary and may spread inaccurate facts.
“Misinformation spreads particularly well on social media because you don’t have professional writers and professional editors controlling what people see,” Bergstrom said. “People just forward things that seem right to them or present a political point of view that they like.”
In addition to holding careers focused in the science aspect of the pandemic, both of these professionals believe mental health and support is important during this time.
“Social distancing doesn’t mean we have to not be there for each
other,” Bergstrom said.
Kauffman hopes UPrep families will use the pandemic as a way to work together and make a difference.
“This pandemic is a life-changing, once-in-a-lifetime event for all of us. It gives us the opportunity to challenge ourselves and be better people who are actively working to preserve the health of our society,” Kauffman said. “Through our compliance with government and public health regulations, our ingenuity, problem solving and our care for those around us, we can all contribute.”
Testing Methods According to Dr. Kauffman
Interested in the methods health workers use to test someone for the coronavirus? Kauffman shared the details of some common testing methods.
“The test for when you’re acutely infected is the swab at the back of the nose… There are some throat swabs and self-swabs that people are doing. That is the best test for people with symptoms for whom we want to find out if they’re acutely ill with the virus,” Kauffman said.
The problem with this method is when you swab someone it is likely that they will cough or sneeze. This makes them more infectious and puts the tester at higher risk. In Seattle and the rest of the country, the tests are hard to get.
“It’s been a pretty significant failure and frustration that we have not had the equipment to test as much as we’d like,” she said.
This makes it more difficult to manage the virus and understand how many people have it. There are many unknowns, like whether the severity of the virus is impacted by the weather or time of year, similar to the flu’s behavior.
However, a new test, called an antibody or serology test, might be an effective way to show how many people have had the virus.
“This is a blood test that doesn’t need personal protective equipment for the tester. This test looks for antibodies to the specific coronavirus that causes COVID-19,” Kauffman said.
The antibody takes time to develop, so a patient may have to wait about 2-4 weeks after they develop symptoms and two weeks after those symptoms go away to actually get good results. In the end, the test will show whether a patient has been infected with the coronavirus or not.
The downside to this method is it is unclear whether or not having the virus once makes someone immune to getting it again. Regardless, this new test is very in demand.

Sydney Goitia-Doran is one of the print editors-in-chief of the Puma Press and she has been on staff for four years. Her favorite types of stories to write...